Gorlin syndrome begins before birth
More than two-thirds of people diagnosed with Gorlin syndrome have a family history of the disease. If a child has one parent with the condition, the odds are 50/50 that the child will also have Gorlin syndrome.
Diagnosing Gorlin syndrome in children
At birth, infants may have features that are characteristic of Gorlin syndrome. These include a larger than normal head size (macrocephaly), prominent forehead (frontal bossing), wide-spaced eyes (hypertelorism), and/or milia below the eyes or on the forehead
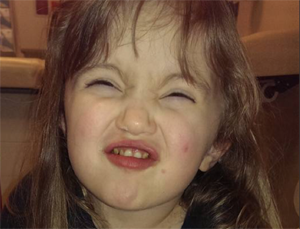
Early diagnosis of Gorlin syndrome is important
Infants and young children with Gorlin syndrome may also be born with cleft palate or cleft lip. There may be problems with the eyes, including very small eyes (microphthalmia), cataracts, rapid involuntary eye movements (nystagmus), missing tissue from the iris or retina (coloboma) and/or crossed eyes (strabismus).
Early diagnosis of Gorlin syndrome is important, especially to monitor and treat BCCs and other abnormal growths. As with adults, Gorlin syndrome is diagnosed in children when the child has at least two major criteria of the condition and one minor, or one major criterion and at least three minor criteria.
Major criteria of Gorlin syndrome:
- Two or more basal cell carcinomas (BCCs) prior to age 30
- Odontogenic keratocystic tumors (OKCs)
- Pitting on the palms and soles
- Calcified falx cerebri or calcium deposits in the brain
- A family history of Gorlin syndrome
Minor criteria of Gorlin syndrome:
- Medulloblastoma, a malignant brain tumor in children
- Large head size and protruding forehead
- Cleft lip or palate, extra fingers or toes
- Abnormally shaped ribs or bones in the spine
- Eye problems such as cataracts, small eyes, or tumors in the iris
- Fibroid tumors in the ovaries or heart
- Abdominal cysts
Childhood signs and symptoms
Of the 100 or so signs and symptoms of Gorlin syndrome, some are present at birth (congenital), and some develop in childhood and continue through to adulthood.
Read more about the signs and symptoms of Gorlin syndrome.
Monitoring Gorlin syndrome in children
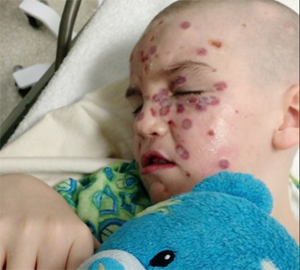
Multiple basal cell carcinomas prior to age 30 are one of the most common symptoms of Gorlin syndrome
Though many of the signs and symptoms of Gorlin syndrome generally do not cause problems for overall health, children with
the condition should have their symptoms regularly monitored by the appropriate health care provider.
Tests to monitor symptoms in children with Gorlin syndrome include:
- MRI of the brain and spine (if scoliosis exists)
- Digital x-rays of jaw
- A full-body skin exam
- Annual hearing, vision and speech evaluations
- Routine well-child visits
- Cardiac ultrasounds (if heart symptoms are present)
- For girls, regular pelvic ultrasounds (if ovarian fibromas are present) starting after first period
- Genetics evaluation
- Psychological exams for emotional health
The child’s health care provider team along with parents/caregivers and the child him or herself should determine the surveillance schedule depending on the presence and severity of symptoms.
Read more about recommended surveillance of Gorlin syndrome symptoms.
Social and developmental issues
Many children with Gorlin syndrome have some delay in motor skill development. However, according to the U.S. National Institutes of Health (NIH), most of them catch up by age 5.
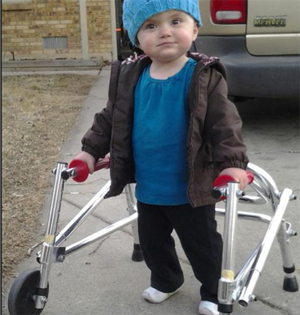
Children with Gorlin syndrome may need therapy to reach certain developmental milestone
Perhaps most challenging for a child with Gorlin syndrome is the physical impact of the disease. Being “different” from his or her peers or siblings can contribute to feelings of anxiety, stress, frustration and sadness in children with Gorlin syndrome.
The American Academy of Pediatrics recommends the following to help your child cope with the challenges of living with Gorlin syndrome:
- Listen to your child and help them express their emotions
- Help your child learn the basics of Gorlin syndrome so that she or he may understand “what lies ahead” with regards to treatment and more
- “Rehearse” potentially frightening situations such as MRIs and other medical tests, so that your child can get a better idea of what to expect
- Encourage your child to spend time with other children who have Gorlin syndrome or other challenging chronic diseases
- Frequently talk about Gorlin syndrome so your child feels more comfortable being open with others about the condition
- Focus on your child’s strengths and help them develop new skills
- Allow your child to feel some control over what is happening to them, i.e. let them decide which arm to draw blood
For school-aged children, it’s a good idea to meet and talk with the teacher about Gorlin syndrome at the start of the school year. A teacher who understands Gorlin syndrome can be a valuable partner to help your child cope in school.
Some children with Gorlin syndrome may benefit from an Individualized Education Plan (IEP) or a 504 plan. Learn the difference between the two and which one you may need.
Emotional wellness

Yours is a child first and a child with Gorlin syndrome second
Feelings of depression, sadness and anxiety, are common in people with chronic disease. According to the National Institute of Mental Health (NIMH), people with chronic medical conditions — such as Gorlin syndrome — are at higher risk of developing depression than those who don’t face serious health issues.
The NIMH states, “It is common to feel sad or discouraged after [your diagnosis] … It may be hard to adapt to a new reality and to cope with the changes and ongoing treatment that come with the diagnosis.”
Temporary feelings of sadness are expected, but if these feelings last longer then a couple of weeks, your child may have depression or another mental health issue.
According to the NIMH, symptoms of depression include:
- Feeling sad, irritable, or anxious
- Feeling empty, hopeless, guilty, or worthless
- Loss of pleasure in hobbies or activities
- Fatigue and decreased energy
- Trouble concentrating, remembering details and making decisions
- Not being able to sleep, or sleeping too much
- Eating too much or not wanting to eat at all
- Thoughts of death or suicide
- Aches or pains, headaches, cramps, or digestive problems without a clear physical cause and/or that do not ease even with treatment
If your child has been experiencing two or more of these symptoms for two weeks or longer, it may be time to talk to a trained professional about these feelings.
Helpful Links for Parents and Caregivers of Children with Gorlin syndrome
Click the logos below to learn more about opportunities for your child. The information below is for general informational purposes only. The Gorlin Syndrome Alliance makes no representation or warranty, express or implied. Your use of the services below is solely at your own risk. The links below are to third party content, which the GSA does not warrant, endorse, or assume liability for. The GSA does not receive remuneration for sharing these links.




